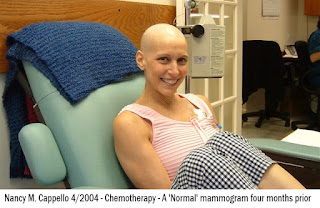From the front-row perspective, younger women are as much at risk of getting cancer. Reports show an uptick in genetic predisposition for breast cancer*, alongside a dangerous attitude of denial. Addressing this calls for widespread education and screening programs in our community as essentials to a life of wellness and prevention. To subscribe to a regular screening routine at the early stage of womanhood raises awareness and prevention for decades to come. Perhaps someday, installing breast cancer screening centers in college campuses may be commonplace and a powerful step toward a national prevention initiative.
From the front-row perspective, younger women are as much at risk of getting cancer. Reports show an uptick in genetic predisposition for breast cancer*, alongside a dangerous attitude of denial. Addressing this calls for widespread education and screening programs in our community as essentials to a life of wellness and prevention. To subscribe to a regular screening routine at the early stage of womanhood raises awareness and prevention for decades to come. Perhaps someday, installing breast cancer screening centers in college campuses may be commonplace and a powerful step toward a national prevention initiative.CURRENT DATA FROM PUBLIC SURVEY Assembled by Dr. Roberta Kline, OBGYN & Co-Editor of Women's Health Digest
Enclosed is research-based public information by the CDC that widely supports the current reality about new cancers (including breast cancer) in women under 40. The data used by public health comes from a wide variety of places within our local communities: hospitals, laboratories, doctors' offices – anywhere that a person receives healthcare. Age-specific rates breast cancer for 2020 (Total for ages 20-39): • Rate of new breast cancers = 27/100,000 • Equals 11,368 new cases/42,765,288 women Details: <20: numbers less than 16 cases for lower age categories, data suppressed 20-24: 1.7/100K; equals 174 new cases/10,239,813 women 25-29: 10.4/100K; equals 1,146 new cases/11,016,549 women 30-34: 30.5/100K; equals 3332 new cases/10,939,868 women 35-39: 63.5/100K; equals 6716 cases/10,569,058 women |
 |
| Click to download the latest ACS report |
 If the drive for EARLIER DETECTION means proactive awareness, may this lead to turning social concern into clinical action. This includes clinicians joining hands with advocacy groups who recognize the many potential areas for at-risk women in my generation whose lives and safety continue to go unrecognized. And once the count of cancer cases and deaths rise exponentially due to inaction, perhaps then will the medical community find urgency in upgrading the required breast cancer screening age to (finally) include generations like mine. So say we all!
If the drive for EARLIER DETECTION means proactive awareness, may this lead to turning social concern into clinical action. This includes clinicians joining hands with advocacy groups who recognize the many potential areas for at-risk women in my generation whose lives and safety continue to go unrecognized. And once the count of cancer cases and deaths rise exponentially due to inaction, perhaps then will the medical community find urgency in upgrading the required breast cancer screening age to (finally) include generations like mine. So say we all!  |
| This article is sponsored by the educational program of Bard Diagnostic Imaging |
Waterbury celebrated a citywide Pink Out on Thursday, October 26th! Saint Mary’s Hospital Foundation has once again partnered with the City of Waterbury to recognize Breast Cancer Awareness. Waterbury Mayor Neil O’Leary, Saint Mary’s Hospital President, Kim Kalajainen and special guest Joe Cappello will address organizers and volunteers from the Waterbury Police and Fire Departments as well as the Education Department, area students and others at 11:00 a.m. at Waterbury City Hall.
Video News Release: Innovations in Early Detection "Are You Dense?" Foundation Co-founder Joe Cappello joins the medical diagnostic community to promote the "Get Checked Now!" campaign. Dr. Robert Bard from the Bard Cancer Center (NYC) supports supplemental imaging including the 3D Doppler Ultrasound scanner to offer dense breast detection. This video presents some of the latest advancements in ultrasound features to detect tumors through dense breast tissue- reportedly a significant challenge with mammograms. |
• Women who are diagnosed with breast cancer at a younger age are more likely to have genetic mutations predisposing them to breast and other cancers.
• Younger women who have breast cancer may ignore the warning signs—such as a breast lump or unusual discharge—because they believe they are too young to get breast cancer. This can lead to a delay in diagnosis and poorer outcomes.
• Some healthcare providers may also dismiss breast lumps or other symptoms in young women or adopt a "wait and see" approach.
• Breast cancer poses additional challenges for younger women as it can involve issues concerning sexuality, fertility, and pregnancy after breast cancer treatment. [1]
3) WHOLE BODY MRI (NO CONTRAST) FOR CANCER SCANNING: In simplistic terms, having a full-body access comports to the fact that everything is connected in one way or another. Our full-body MRI provides early diagnosis and the largest view of the body, where finding any cancers in the body and/or where they may spread can provide the best chance of treatment success. In suspected cases of early breast malignancy, the exclusion of metastatic disease is clinically vital and emotionally supportive.
1a) "Infographic: 7 Things to Know About Getting a Mammogram"- ACA/American Cancer Society: https://www.cancer.org/cancer/types/breast-cancer/mammogram-tips-infographic.html#:~:text=Women%20between%2040%20and%2044,choose%20to%20continue%20yearly%20mammograms.
1) "Breast Cancer in Young Women"- Cleveland Clinic: https://my.clevelandclinic.org/health/articles/16805-breast-cancer-in-young-women
2) "What additional breast cancer screening tests are available for women who have dense breasts?"- Yale medicine- https://www.yalemedicine.org/conditions/dense-breasts#:~:text=Women%20diagnosed%20with%20dense%20breasts,(whole%2Dbreast%20ultrasound).
3) Columbia Doctors/ "What Are Dense Breasts? A radiologist offers guidance":-Health Insights: October 14, 2022 https://www.columbiadoctors.org/news/what-are-dense-breasts#:~:text=Any%20woman%20who%20has%20dense,in%20women%20with%20dense%20breasts.